Neonatology
Session: Neonatal Neurology 6: Clinical
557 - Intrauterine temperature during intrapartum amnioinfusion for neuroprotection: Secondary analysis of a pilot randomized trial
Saturday, May 4, 2024
3:30 PM - 6:00 PM ET
Poster Number: 557
Publication Number: 557.1535
Publication Number: 557.1535
- BP
Brock E. Polnaszek, MD (he/him/his)
Maternal Fetal Medicine Fellow
Women & Infants Hospital of Rhode Island, Warren Alpert Medical School of Brown University
Providence, Rhode Island, United States
Presenting Author(s)
Background: Amnioinfusion is a common obstetric intervention in which room temperature saline is infused into the uterus. Since it is well known that cooling in the setting of HIE reduces neonatal morbidity postnatally, intrauterine temperature (IUT) may impact neonates at risk during labor. The effect of amnioinfusion on IUT has not been examined in a randomized trial.
Objective: We aimed to analyze the effects of room temperature amnioinfusion on intrapartum IUT.
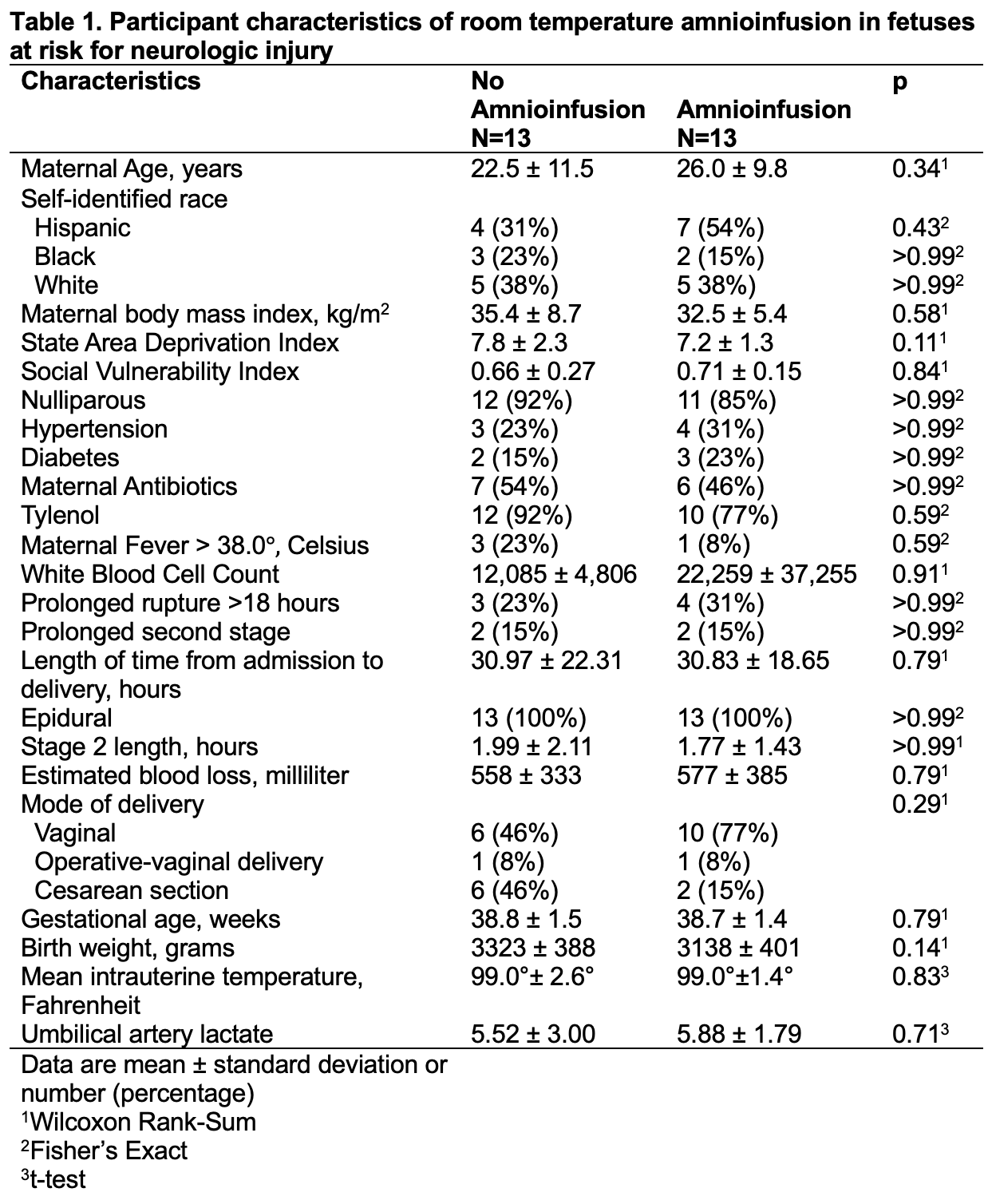
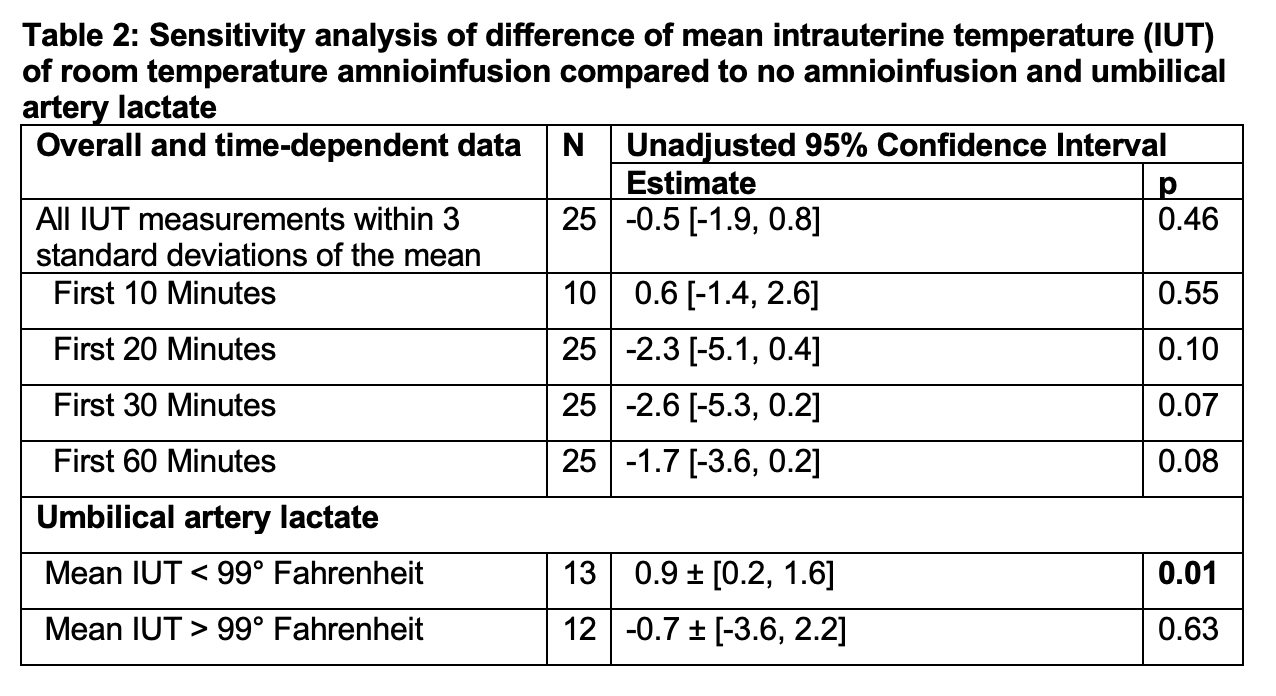
Design/Methods: A recent pilot randomized trial examined the effect of intrapartum amnioinfusion on term, singleton pregnancies who developed risk factors for fetal neurologic injury such as chorioamnionitis or Category 2 fetal heart rate tracing (NCT05513690). Participants underwent intrauterine pressure catheter placement and randomization to continuous room temperature amnioinfusion or no amnioinfusion. Room temperature amnioinfusion was administered with a bolus of normal saline over one hour, followed by a maintenance rate until delivery. IUT was monitored every 10 minutes with an IUT probe (DataTherm II, Medline) from randomization. For this secondary analysis, participants were excluded if IUT data were more than three standard deviations from the randomized cohort mean, as no established IUT distribution exists. To isolate the effect of amnioinfusion bolus administration on IUT, differences in mean IUT were analyzed for the first 10, 20, 30, 60 minutes and overall time between groups. Participants were further dichotomized by IUT above or below the mean and analyzed for the effect on umbilical artery lactate—a validated surrogate of fetal tissue ischemia.
Results: Among 26 participants (Table 1) in the primary trial, the mean IUT was 99.0±[standard deviation 2.1]° Fahrenheit and was not different between groups. Among the 25 participants (95.4%) included in this secondary analysis, IUT was lower with amnioinfusion for the majority of time points (e.g. differences in mean IUT -2.6 [-5.3, 0.2]° first 30 minutes, p=0.07), although not statistically significant. Among participants dichotomized below the mean IUT, an increase of IUT by one degree raised umbilical artery lactate estimate 0.9 [95% CI 0.2, 1.6], p=0.01.
Conclusion(s): Despite no statistical difference in IUT regardless of amnioinfusion, these pilot data support a pathway between intrapartum amnioinfusion, IUT, and umbilical artery lactate. Future randomized trials should identify the optimal amnioinfusion technique (e.g. cooled fluids) which may allow clinicians to reduce the risk of neurologic injury in utero.