Hospital Medicine
Session: Hospital Medicine 5
145 - Antibiotic Route and Outcomes for Children Hospitalized with Pneumonia at 43 Children's Hospitals
Saturday, May 4, 2024
3:30 PM - 6:00 PM ET
Poster Number: 145
Publication Number: 145.1622
Publication Number: 145.1622

Jillian Cotter, MD, MSCS
Pediatric Hospitalist
University of Colorado / Children's Hospital Colorado
Aurora, Colorado, United States
Presenting Author(s)
Background: Emerging evidence suggests that initial oral and intravenous (IV) antibiotics may have similar efficacy for children hospitalized with community-acquired pneumonia (CAP), but further data are needed.
Objective: We identified hospital-level rates of initial treatment with oral antibiotics and evaluated the association between hospital-level initial oral antibiotic treatment rates and clinical outcomes.
Design/Methods: This retrospective cohort study included hospitalized children (3 months-18 years) treated with antibiotics for CAP at 43 hospitals within the Pediatric Health Information System from 2016-2022. Encounters were identified as receiving initial oral vs. IV treatment based on the antibiotic route given on the first hospital day. Hospitals were grouped according to whether initial treatment with oral antibiotics occurred in a high, moderate, or low proportion of patients using the outlier status approach. Multivariable regression models examined associations between high vs. low oral-utilizing hospitals and length of stay (LOS) as well as secondary outcomes including intensive care unit (ICU) transfer, escalated respiratory care (receipt of high flow oxygen or non-invasive positive pressure ventilation), complicated CAP diagnosis, cost, 7-day CAP-related readmission or ED-revisits, and readmissions for complicated CAP.
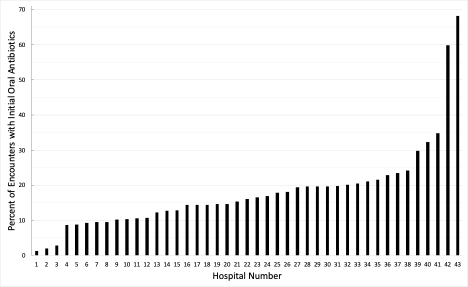
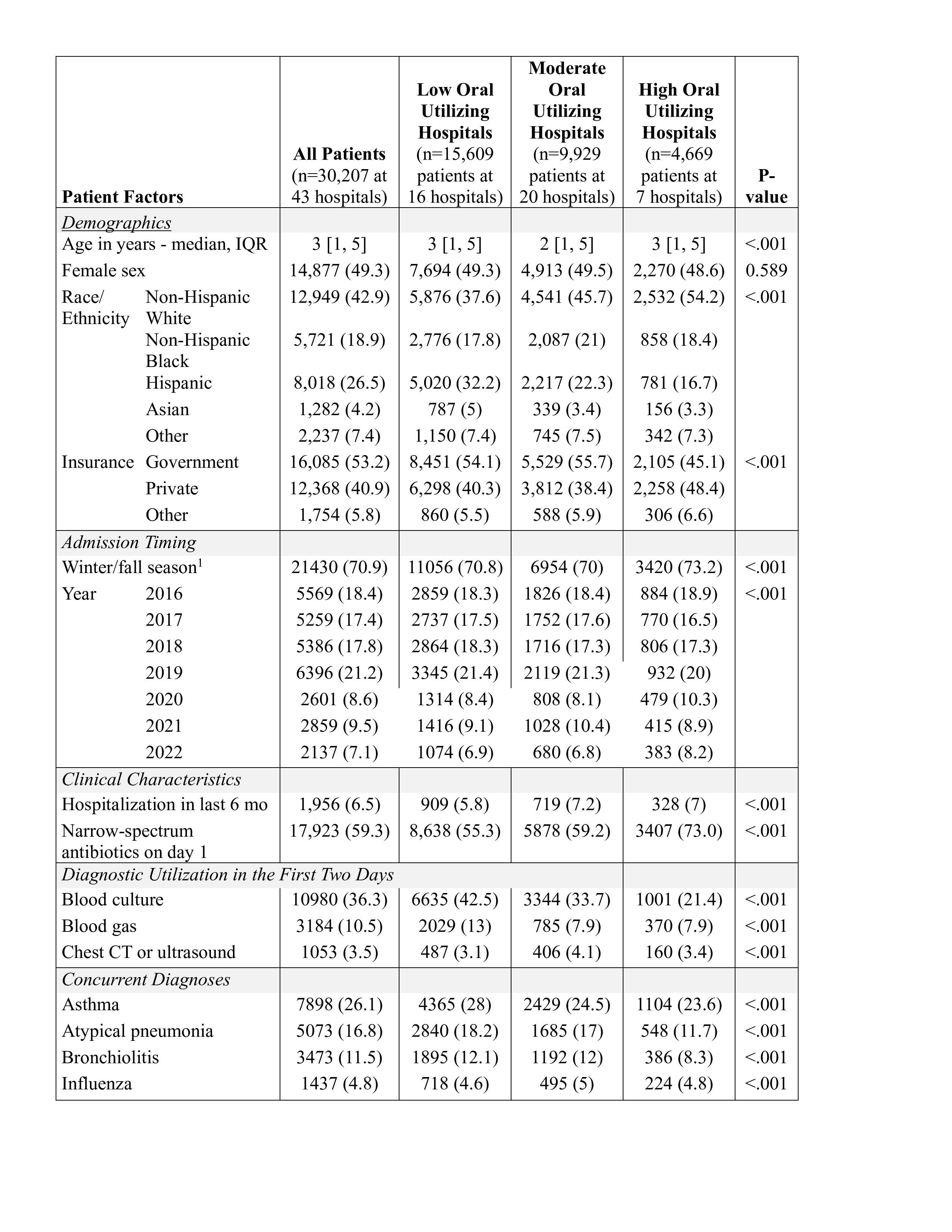
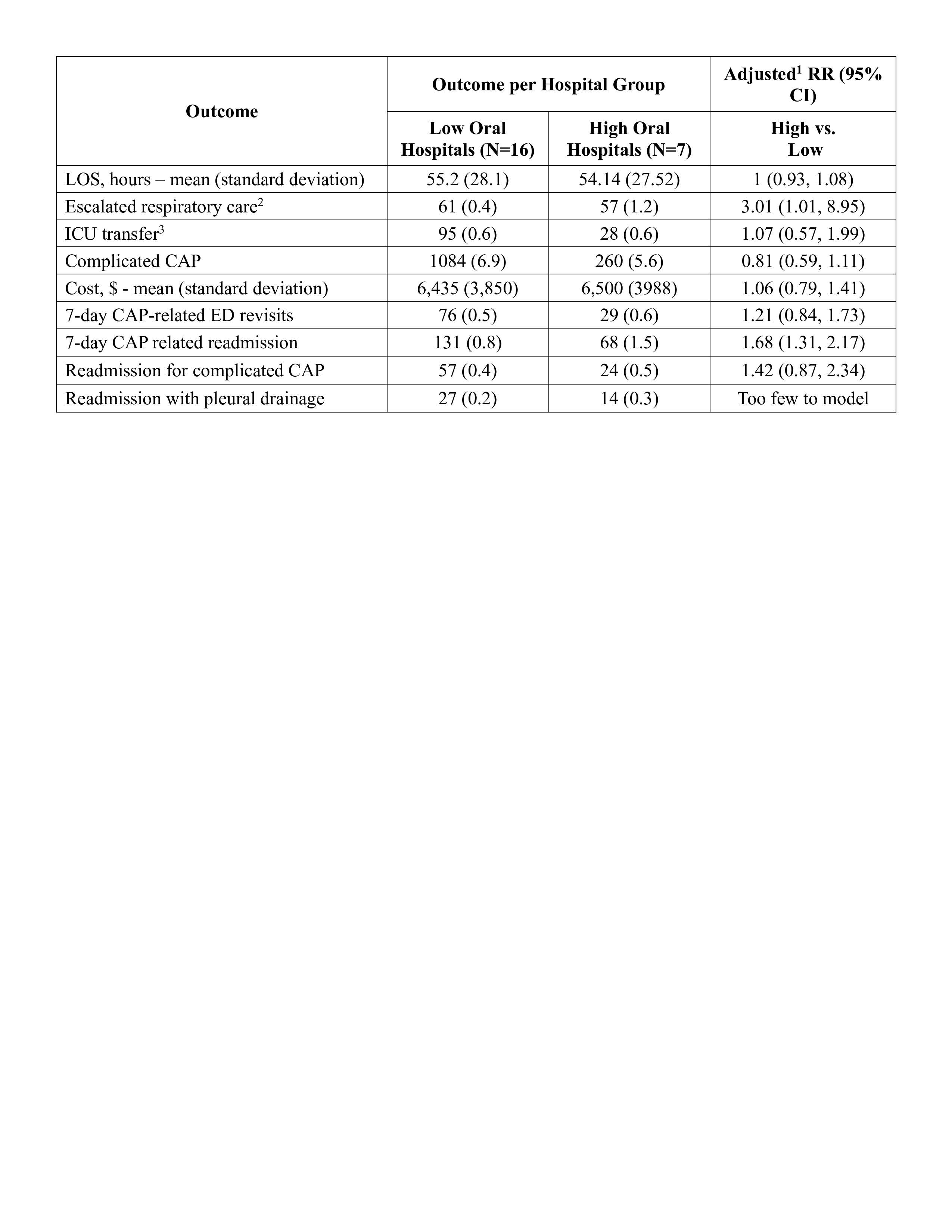
Results: Of 30,207 encounters, initial oral antibiotics were utilized in 16% (IQR 10-20%) of encounters, ranging from 1-68% across hospitals (Figure 1; Table 1). When comparing high vs. low oral-utilizing hospitals (median oral rate: 32% [IQR 27-47%] and 10% [9-11%], respectively), there was no difference in LOS (Table 2). High oral-utilizing hospitals had a higher rate of escalated respiratory care (1.2% vs. 0.4%, RR 3.01 [1.01, 8.95]) and CAP-related readmissions (1.5% vs. 0.8%, RR 1.68 [1.31, 2.17]). However, there were no differences in other secondary outcomes including ICU transfers or readmissions for complicated CAP.
Conclusion(s): The use of initial oral antibiotics varied widely across hospitals, highlighting the need to identify and disseminate best practices. Rates of initial oral antibiotic use were not associated with differences in LOS. While high initial oral antibiotic hospitals had a statistically higher rate of respiratory care and readmissions, these outcomes were rare, the clinical significance of these small absolute differences is uncertain, and there were no differences in other clinically relevant outcomes. These results suggest that a subset of children may benefit from initial IV antibiotics, but many others would likely do well with oral therapy.