Neonatology
Session: Neonatal General 3: Maternal and Fetal Medicine
88 - Value of Umbilical Cord Screening for Detection of Fentanyl Exposure During Prenatal Period
Friday, May 3, 2024
5:15 PM - 7:15 PM ET
Poster Number: 88
Publication Number: 88.219
Publication Number: 88.219
- DR
Divya Rana, MD
Associate Professor
University of Tennessee Health Science Center College of Medicine
University of Tennessee Health Science Center
Memphis, Tennessee, United States
Presenting Author(s)
Background: Illicit fentanyl has emerged as a significant etiology of all opioid overdose deaths in the US with a six-fold increase from 2015 to 2020. The illegally used fentanyl is added as a powder, dropped onto blotter paper, put in eye droppers and nasal sprays, or made into pills that look like other prescription opioids. Some drug dealers are mixing fentanyl with other drugs, such as heroin, cocaine, methamphetamine, and 3,4-Methylenedioxymethamphetamine (MDMA), commonly known as ecstasy. This is especially risky when people taking drugs don’t realize they might contain fentanyl.
Objective: To assess the risk of neonatal opioid withdrawal syndrome with prenatal illicit fentanyl exposure with negative maternal self-report of fentanyl.
Design/Methods: This is a Cross-sectional cohort study of neonates born to mothers with evidence of opioid abuse from January 2018 to December 2022. Maternal substance use was confirmed with a positive urine toxicology and an umbilical cord (UCT) testing. We utilized UCT 17-panel that also screens for Fentanyl since March 2020. Infant and maternal demographics, enrollment in opioid maintenance program (OMP) were recorded. We defined severe NOWS as a need for pharmacological treatment and a Mild/no NOWS without such treatment.
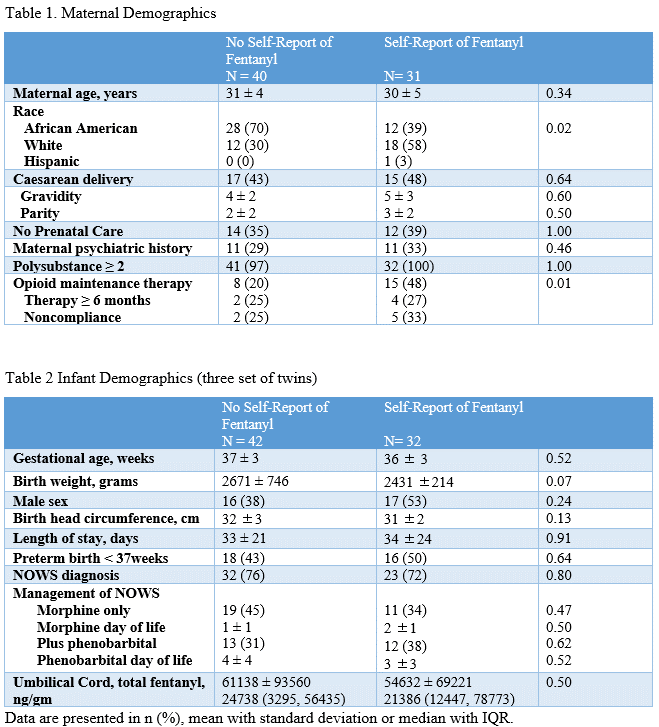
Results: During study period, 45% [155/347] mothers had evidence of opioid use disorder (OUD). Among the 160 infants born to these mothers, 46% (74/160) screened positive for fentanyl. However, 57% [42/74] had no report of fentanyl use during pregnancy but infant’s umbilical cord tested positive for fentanyl metabolites. Figure 1 demonstrates the rising rate of fentanyl with concomitant decrease in other forms of opioids, including heroin. Maternal and infants’ demographics based on maternal self-report of fentanyl are shown in tables 1 and 2. In general, we have older mothers with poor prenatal care and polysubstance use. Even though more mothers who reported fentanyl use were enrolled in OMP, only 25% were able to stay in program for 6 months or more. Fentanyl exposure remained significant risk for severe NOWS in both groups and overall OR 8.3 [CI95 4.4, 15.6], p < 0.01. The NOWS presentation on average in both groups was within 2 days of birth; and up to 35% infants requiring combination therapy with phenobarbital within first week of life.
Conclusion(s): Among Mothers with OUD there is a recent significant increase for fentanyl use with subsequent risk for severe NOWS. Mothers have low self-report for fentanyl abuse and be misleading for neonatal care.